You made it through your teen years, and at some point your skin probably stopped being the main character in your life. No more intense treatment, no more specialty products.
So when pimples start showing up again as an adult it can feel both surprising and discouraging. The reaction is often the same: I’m taking better care of my skin now. Why is this happening?
That question is the right place to start, because adult acne usually isn’t a sign that you’ve suddenly done something wrong. More often, it’s a sign that something about your skin’s environment has changed. Once you understand what tends to change in adulthood, the path forward becomes much clearer.
This is a good reason why you should speak to a dermatologist about persistent or recurring adult acne. The research on adult acne has only grown in recent years, and dermatologists are becoming better not only at managing it, but also in treating it (and the scars it can leave behind).
First things first: Are you sure it’s acne?
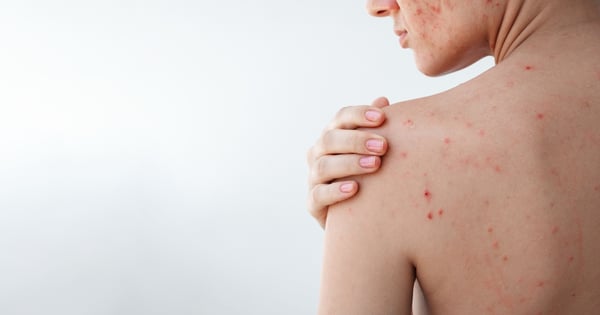
When new bumps appear, it is natural to assume they are acne. But several skin conditions can mimic breakouts so closely that even experienced patients sometimes misidentify them. For example, folliculitis can resemble acne, often presenting as clusters of uniform, itchy bumps. Rosacea may create persistent redness and sensitivity that flare with certain triggers. And perioral dermatitis typically shows up as a rash-like eruption around the mouth or nose and can worsen with heavy products or topical steroids.
A simple way to think about it is this: Acne is primarily a clogged-pore problem (often with inflammation on top). Many other conditions also create bumps, but for entirely different reasons. If you treat folliculitis, rosacea, or perioral dermatitis like acne, you can end up drying and inflaming your skin, which will make the original issue more persistent and harder to treat.
Here are a few clues that it may be something other than classic acne:
- Bumps are very uniform and itchy, especially in clusters
- You see persistent background redness or flushing along with sensitivity
- Breakouts concentrate around the mouth or nose and feel rash-like
- Acne products seem to make your skin more inflamed, not calmer
All of that said, guessing which condition you have by trial-and-error tends to backfire. Skin rarely responds well to rapid product changes, particularly when inflammation is involved. A dermatologist can usually distinguish among these various conditions quickly and recommend targeted treatment, sparing you months of guesswork.
Understanding what adult acne is (and how it’s different from teen acne)
Adult acne is extremely common. In fact, the American Academy of Dermatology notes that acne is one of the most common diseases worldwide, and often persists into adulthood.
That said, adult acne isn’t just teen acne that didn’t get the memo. It’s often driven by a combination of factors that are more common later in life: hormonal fluctuations, friction and occlusion, changes in the skin barrier, and lifestyle stressors that impact inflammation.
So before you ask “What product should I buy to treat this?” it’s usually more helpful to ask: “What changed in my skin’s biology or daily conditions that makes breakouts more likely now?”
Here are some of the most common answers to that question.
Hormones still influence your oil glands
Hormones don’t stop affecting skin once adolescence ends. For many women, adult acne clusters around the jawline and chin and tends to flare with menstrual cycles, postpartum shifts, or perimenopause. For others, stress hormones play a role by nudging oil production and inflammation upward.
The important point isn’t that acne is “all hormones.” It’s that hormones can create a baseline tendency toward clogged pores—and then other factors determine whether those pores turn into visible breakouts.
Friction and occlusion are more common in adult life
Adult routines include items that constantly trap heat, sweat, and oil against the skin. Think workout headbands, helmets, masks, tight collars, phone screens, even certain pillows or hair products. These things aren’t bad for you, but they can introduce rubbing (friction) and clogging (occlusion) that in turn becomes acne. (Dermatology literature describes this pattern as acne mechanica, a form of acne driven primarily by pressure, friction, occlusion, and heat acting on the skin. It is common, for example, in athletes and other people who are active.)
When adults say, “My skin used to tolerate anything,” what they often mean is that their skin used to recover faster from these inputs. Over time, that “tolerance” can change.
Your skin barrier may be failing—without you realizing it
Your skin barrier is the outermost layer of skin that keeps moisture in and irritants out. When it’s healthy, it acts like a protective seal, helping your skin stay calm and resilient even when exposed to bacteria, sweat, or environmental stress.
Many adults unintentionally disrupt that barrier while trying to control breakouts. The instinct is understandable: When pimples appear, it feels logical to cleanse more often, exfoliate aggressively, skip moisturizer, or layer multiple treatment products at once.
But skin that is repeatedly stripped becomes dry and microscopically cracked. Those tiny disruptions allow irritants to penetrate more easily and trigger inflammation (one of the key processes behind acne). At the same time, overly dry skin can signal oil glands to compensate by producing more oil, creating conditions where pores are more likely to clog.
This is why breakouts sometimes seem to worsen just as someone becomes more disciplined about skincare. It’s not that treatment is a mistake—it’s just that the skin is being pushed faster than it can repair itself.
Lifestyle doesn’t “cause” acne…but it can keep it going
Sleep disruption, stress, travel, and inconsistent routines don’t create acne out of nowhere. What they often do is keep your skin from stabilizing. When your routine changes every few days (or when you’re under sustained stress) the skin barrier tends to suffer, inflammation rises, and acne can become more persistent.
That’s why adult acne so often feels like it appears “for no reason.” The reasons aren’t always dramatic. They’re cumulative.
Building a consistent routine with time to repair
Skin tends to improve more through consistency, not intensity. The best thing to do for adult acne (outside of seeing your dermatologist) is to create a routine that supports the skin barrier and reduces baseline inflammation.
Start with three essentials: a gentle cleanser, a lightweight non-comedogenic moisturizer, and daily sunscreen. While simple, this foundation allows your skin to function normally—which in turn makes any treatment you introduce more effective and less irritating.
Once your routine is steady, introduce one proven treatment rather than several at once. Retinoids, benzoyl peroxide, and salicylic acid can all help, but layering them too quickly frequently leads to dryness that complicates the picture instead of clarifying it.
Expect progress to unfold over weeks, not days. Adult skin rarely responds well to abrupt changes, but it often improves reliably with steady care.
When it makes sense to involve a dermatologist
If breakouts remain deep, painful, persistent, or are beginning to scar, having the help of a board-certified dermatologist can be a game changer. This is less about trying something “stronger” and more about choosing something more precise.
Dermatologists evaluate patterns, triggers, and skin behavior to design a plan that fits your situation. Depending on your needs, treatment may include prescription topical medications, targeted anti-inflammatory therapies, or hormonal options for appropriate patients. There are also a number of advanced treatments that have come out in just the last year or so, such as bacteriophage acne therapy, photodynamic therapy (PDT), and fixed-dose combination topicals.
When acne treatment matches what your skin is actually doing, improvement typically becomes more predictable and far less frustrating.
The bottom line
Adult acne is not a personal failure, and it is not uncommon. In most cases, it’s the result of ordinary shifts in hormones, barrier health, friction, and lifestyle stress. Those kinds of changes happen to many adults at some points in their lives.
The response should be clear diagnosis, a stable skincare routine, and if needed, a treatment plan that matches what your skin is actually doing.
A board certified dermatologist can help with any or all of these steps. Use our location finder to find a Forefront dermatologist near you.