Now that masks are here to stay, well hopefully they aren’t here forever… some mask wearers are noticing that regular mask use is leading to flare-ups of certain skin conditions including eczema and rashes. Some individuals are even seeing that the result of a warm, moist environment trapped in a mask is leading to fungal acne.
What is fungal acne?
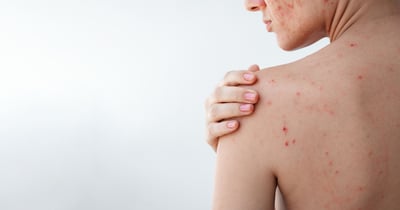
According to Dr. August Natalie, board-certified dermatologist with Forefront Dermatology, “Fungal acne is also known as fungal folliculitis. It occurs when yeast enters the hair follicle and multiplies, causing acne-like breakouts on the skin’s surface. Sometimes you will notice these papules as pink, but they occasionally will have a whitehead. It is also common to experience redness, swelling, itching and the occasional stinging sensation.” Fungal acne can occur anywhere that the environment is warm, moist, and has creased skin. Under the perfect combination of factors, the area under your COVID-19 mask can develop into an infection. The skin creases around your mouth and nose, likely due to aging, are a common place for fungal acne to thrive. Individuals with oiler skin types and those prone to acne, eczema, and rosacea flare-up are more likely to develop a potential infection.
How do I know if I have COVID-19 fungal acne?
If you are noticing small, raised blisters, pimples, rash, soreness, and chafing, please seek assistance from a board-certified dermatologist immediately. Delayed treatment can lead to a worsened infection. Treatment is typically a topical product that will help treat the infection within 7 to 10 days.
How can I prevent fungal acne and COVID-19 mask ance?
To prevent fungal acne and COVID-19 mask acne, the best thing you can do is wear a mask that uses a breathable fabric, like cotton. Regularly wash your masks in a gentle detergent to prevent further irritation. If possible, rotate masks throughout the day. Dr. Natalie states, “Outside of wearing a clean mask, simply developing a regular morning and nighttime skincare routine with a gentle cleanser and moisturizer is the best fungal acne prevention. The dirt, oil, and bacteria get trapped under the mask and can cause breakouts, or maskne as people are referring to it as.”
What is the best fungal acne treatment?
Fungal acne treatment is as simple as the preventative process – a twice-daily skin cleansing routine. Check your skincare products, including makeup, to make sure they are non-comedogenic. “Fungal acne treatment, and mask acne treatment, begin with being consistent in the care of your skin and the use of your masks. Do not expect acne to clear up the day after you start a routine,” added Dr. Natalie. “Give it a few weeks of consistent care to start seeing changes. If your acne worsens, you may need a topical or oral prescription.
Suffering from fungal acne?
We recommend that anyone with new or worsening acne loss seek out help from a board-certified dermatologist to determine the underlying cause and find the best course of treatment to fit your lifestyle. Find a dermatologist near you today.

Book an appointment with your trusted, local dermatologist.